"
Updating
your models and predictions in light of new evidence and new
inferential methods and insightful counterpoints from colleagues isn't
a sign of weakness, it's *doing science*. We don't stake out positions
on day 1 and then defend them as if our reputation depends on it.
Rather, reputations depend on being flexible in light of new findings.
You don't drop an idea just because it is criticised; you fight for it.
But you also walk away when it's time."
--
Carl T Bergstrom
"
This virus does have the ability to transmit far easier than flu.
It's probably now about three times as infectious as flu. One of the
[pieces of] information that we have pretty much confirmed now is that
a significant number of individuals that are infected actually remain
asymptomatic. That may be as many as 25%. That's important, because now
you have individuals that may not have any symptoms that can contribute
to transmission, and we have learned that in fact they do contribute to
transmission. And finally, of those of us that get symptomatic, it
appears that we're shedding significant virus in our oropharyngeal
compartment, probably up to 48 hours before we show symptoms. This
helps explain how rapidly this virus continues to spread across the
country, because we have asymptomatic transmitters and we have
individuals who are transmitting 48 hours before they become
symptomatic."
--
Robert Redfield, US CDC Director (see also:
aerosol transmission of SARS-CoV-2)
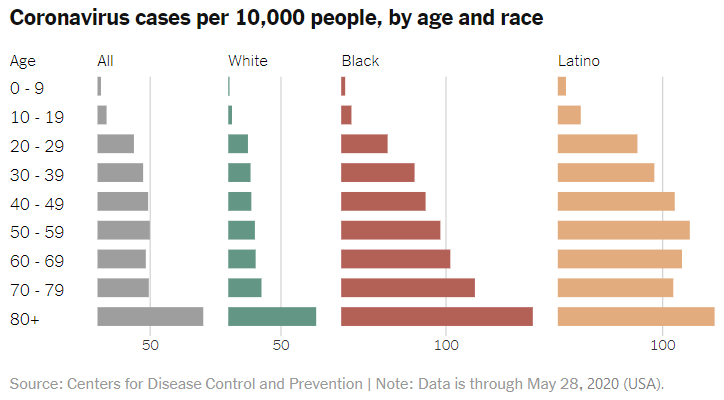
This is
not like seasonal flu:
Significant numbers of young people, but also
some teenagers (12-19),
can and do become critically unwell and die from COVID-19. A review of
more than 4,000 US patients who were diagnosed with COVID-19 shows that
an unexpected
20% of deaths occurred among adults aged 20-64 years, and
20% of those hospitalised were aged 20-44 years, increasing to 40% when
age range is extended to 54 (20-54 years) (Source: Severe Outcomes
Among Patients with Coronavirus Disease 2019 (COVID-19) — United
States, February 12–March 16, 2020.
MMWR
Morb Mortal Wkly Rep 2020;69:343-346. DOI:
http://dx.doi.org/10.15585/mmwr.mm6912e2).
The
US CDC also researched 49,000 coronvavirus cases between February 12
and April 9, 2020, and found that 9,300 of them, 19%, involved
healthcare workers.
SARS-CoV-2
is unusual in that it manages to block the interfeon-I and III response
quite thoroughly, while setting off a larger-than-normal cytokine
secretion response. (If you add IFN-I back to the infected cells in
culture, they clear the virus very strongly – the machinery is working,
but it is just not being engaged.)
COVID-19 mortality might be due to virus-activated
'cytokine storm syndrome' (but see
here) or
fulminant myocarditis (
cardiac injury) or
abnormal clotting (hypercoagulation) and
endotheliitis across different organs.
Silent hypoxia might be a reason why so many early cases are missed until they become severely complicated or fatal. In infants and children:
PIMS-TS.
Transplacental transmission of SARS-CoV-2 infection has been documented. There is also evidence of
persistent symptoms in many patients after acute COVID-19. In July 2020, UK neurologists published details of
mildly affected or recovering Covid-19 patients with serious or potentially fatal brain conditions. There is also mounting evidence that herd immunity to Covid-19 is 'unachievable':
a,
b.
"Immunity can be incomplete, it can be transitory, it can last for just
a short time and then disappear," Raquel Yotti, the director of Spain's
Carlos III Health Institute,
said. Related:
T-cell immunity with SARS-CoV-2 and the
Nsp1 protein of SARS-CoV-2.
See also:
Complications from COVID-19 may depend on von Willebrand factor in the blood and
other genetic factors that may influence COVID-19 susceptibility.